Natural Pain Relief for Joint Pain with No Side Effects
Caviarlieri | Published June 09, 2021
Joint Pain Is a Common Denominator
There are two types of Arthritis.One of them is caused by inflammation and is known as rheumatoid arthritis (RA), and the other caused by normal wear and tear of our joints over years of use and is known as osteoarthritis. Both are often characterized by joint-related symptoms. “Pain involving joints — knees, hips, wrists — indicates the problem is arthritis,” explains Andrew D. Ruthberg, MD, assistant professor of medicine in the division of rheumatology at Rush Medical College in Chicago. Back pain, neck pain, and joint swelling are also markers of arthritis.
What Osteoarthritis Pain Feels Like
Here are some common signs and symptoms of osteoarthritis pain:
- Pain that aches deep into the joint
- Pain that gets worse throughout the day
- Joint pain that affects your posture and gait and may cause limping
- Pain that occurs after using the joint and there is swelling in the joint
What Rheumatoid Arthritis Pain and Discomfort Feels Like
Rheumatoid arthritis, or RA, is an autoimmune and inflammatory disease, which means that your immune system attacks the healthy cells in your body by mistake, causing inflammation (painful swelling) in the affected parts of the body
Since rheumatoid arthritis is a chronic inflammatory disease, it will progress aggressively if it is not treated early. According to a study published in a 2018 issue of the Journal of the American Medical Association, “Early diagnosis and treatment of RA can avert or substantially slow progression of joint damage in up to 90 percent of patients, thereby preventing irreversible disability.”

Rheumatoid arthritis symptoms often Include More Than Joint Pain
- Joint pain that occurs on both sides of the body, such as both feet, ankles, wrists, or fingers
- Significant stiffness in the morning that persists for at least an hour
- Aching muscles all over the body and weak muscles
- Feeling tired or depressed
- Pain that will ease for periods, then get significantly worse, rather than consistent pain
- Heat and soreness in the joints
Where to turn for pain relief – acetaminophen or NSAIDs?
The first line of treatment for many knee and hip problems includes taking over-the-counter pain medications. Acetaminophen and non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen are the most common pain medication options.
Acetaminophen (Tylenol and other brands) is usually effective for mild pain and is easy on the stomach. However, it is toxic to the liver at high doses.
How do painkillers work?
NSAIDs work by blocking (inhibiting) the effect of chemicals (enzymes) called cyclo-oxygenase (COX) enzymes. COX enzymes help to make other chemicals called prostaglandins. Some prostaglandins are involved in the production of pain and inflammation at sites of injury or damage. A reduction in prostaglandin production reduces both pain and inflammation.
Paracetamol – no one really knows for sure exactly how paracetamol works. But it is also thought to work by blocking COX enzymes in the brain and spinal cord (central nervous system). Paracetamol is used to treat pain and to lower a high temperature. However, it does not help with inflammation.
Opioids work by binding to certain receptors (opioid receptors) in your central nervous system, your gut and other parts of your body. This leads to a decrease in the way you feel pain and your reaction to pain, and it increases your tolerance for pain.
Adverse Side Effects of Painkillers

NSAID medications have side effects, the most common is stomach irritation. It can also cause stomach and intestinal ulcers, which can lead to internal bleeding. NSAIDs also carry an increased risk of heart attack, stroke, and kidney failure when taken at high doses or for long periods of time.
Opioids are strong drugs and they are not the best way to treat long-term or chronic pain, such as arthritis, low back pain.
Over time, the body gets used to opioids and they stop working as well. To get the same relief, you need to take more and more. This is called “tolerance.” Higher doses can cause serious side effects:
NSAID Side Effects:
- Nausea, vomiting
- Constipation
- Not being able to urinate (empty your bladder)
- Slowed breathing, which can be deadly
- Confusion and mental disturbance
Opioids can be addictive. Long-term use of opioids can lead to “physical dependence” – if you stop using them abruptly, you will experience withdrawal symptoms, such as strong cravings, sweating, muscle aches and insomnia. People who take opioids long-term can become addicted, sometimes with dangerous results.
Other Non Drug treatments may work better and have fewer risks.

- Massage therapy/ Acupuncture
- Injections (such as steroids) – Steroid injections can help reduce pain in affected joints. However, they should not be used repetitively because they can cause additional joint damage over time.
- Ultrasound, phonophoresis, and iontophoresis – Therapeutic ultrasound is a simple procedure that uses sound waves to increase blood flow, relax muscle spasms, and aid healing that leads to faster hip pain relief and knee pain relief.
Iontophoresis uses electrical currents to speed the delivery of medication to damaged tissue, or simply to reduce muscle spasms and related irritation - Therapeutic exercise – Strengthening the muscles around a damaged knee or hip can help reduce stress on a joint. The proper balance of strength in the muscles can hold the joint in the most functional and least painful position. Flexibility exercises (to stretch and relax specific muscles) are also an important part of an exercise plan to improve joint function.
Supplements for Joint Pain
There are also dozens of supplements that claim to treat joint pain, but which ones actually work?
Some of the popular supplements are turmeric, fish oil, glucosamine, chondroitin etc.
Despite a lack of conclusive scientific evidence that these supplements can help improve joint pain, they are touted not only as arthritis pain relievers but also as treatments to prevent joint disease.
Yet, a number of past studies have come to mixed conclusions — some studies found that people felt better taking glucosamine and/or chondroitin, but at least as many have found no benefit. A 2010 analysis of multiple studies (called a meta-analysis) found that among more than 3,800 people with osteoarthritis of the knee or hip, treatment with glucosamine, chondroitin, or the combination was no better than placebo. The case for these supplements protecting joint health or preventing arthritis is similarly weak.
Try Caviarlieri – Swiss Caviar Cellular Therapy Food Supplement

Caviarlieri is a Swiss Caviar Food Supplement formulated with the finest Caviar Cellular Extracts and marine peptides and highly polymerized collagen which have strong anti-inflammatory properties that can help alleviate and reduce chronic joint pain significantly.
Unlike painkillers or opioids which have adverse side effects, Caviarlieri is an excellent nutritional supplement which has no side effects and is a great palliative for chronic pain management. Scientific studies of Caviarlieri published in peer reviewed journals have demonstrated that its primary bio active ingredient, Caviar DNA Extract is more effective than taking DHA and its positive results become more significant over time (18 weeks).
Empirical randomised double-blind placebo studies of the key ingredients of Caviarlieri also show outstanding results for knee osteoarthritis and back pain. In the clinical studies findings, it was found that Caviarlieri is also able to reduce the Tumour Necrosis Factor Alpha which is an important inflammatory biomarker for arthritis and fibromyalgia. There are also several ongoing studies which indicate that Caviarlieri triggers the epigenetic mechanisms of the cells to activate gene expression for inflammation reduction.
A. Effective Treatment for Osteoarthritis With No Side Effects
Osteoarthritis is the most common form of arthritis, affecting millions of people worldwide. It occurs when the protective cartilage that cushions the ends of your bones wears down over time. It is a progressive chronic disease that can lead to impaired joint function and can result in excruciating pain and disability.
- Published in Peer Reviewed Journal – Acta Bio Medical / Official Journal of the Society of Medicine and Natural Sciences of Parma Vol 84-N1/2013
Testing a novel bioactive marine nutraceutical (Caviarlieri) on Osteoarthritis patients
This study highlights the effect of Caviar DNA extract (LD-1227) on MMPs, collagen metabolism and on chondrocyte inflammatory markers. The primary objective of the study was to test the effectiveness of the Caviar bioactive compound versus a common nutraceutical intervention like GC (glucosamine/chondroitin sulphate) in knee osteoarthritis patients. The patient population involved in the study consisted of 60 subjects who had a recent diagnosis of knee osteoarthritis of mild-moderate severity. The patients were randomized in two groups in a double-blind study comparing Caviar Extract LD-1227 (group A) versus a mixture of glucosamine (500 mg), chondroitin sulphate (400 mg) (group B). Patients were allowed their established painkillers on demand. At 4, 9 and 18 weeks patients were evaluated based on various validated pain score systems like VAS score which assesses pain at rest, and during physical exercise, Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) scale and KOOS scale.
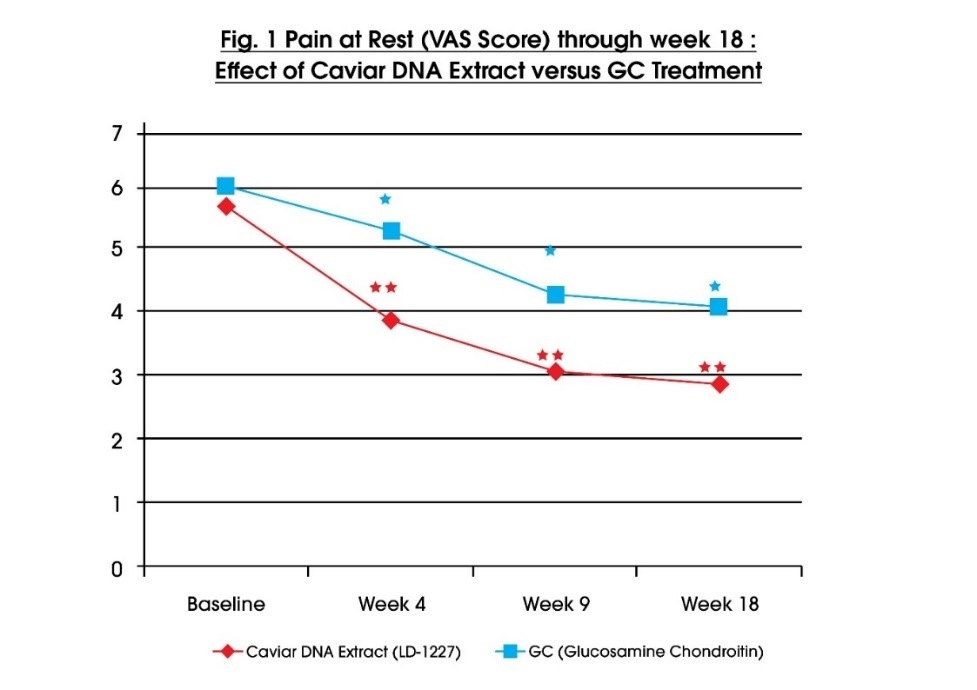
It is evident from the above figure 1 that after 4 weeks, patients treated with Caviar DNA extract (LD1227) showed a decline in VAS Score (p<0.05) which means that the pain (at rest) for these patients is significantly lower than those treated with Glucosamine Chondroitin (GC).
Note: VAS Score is a 0-100mm Visual Analog Scale Score system which assesses pain during the most painful knee movement.
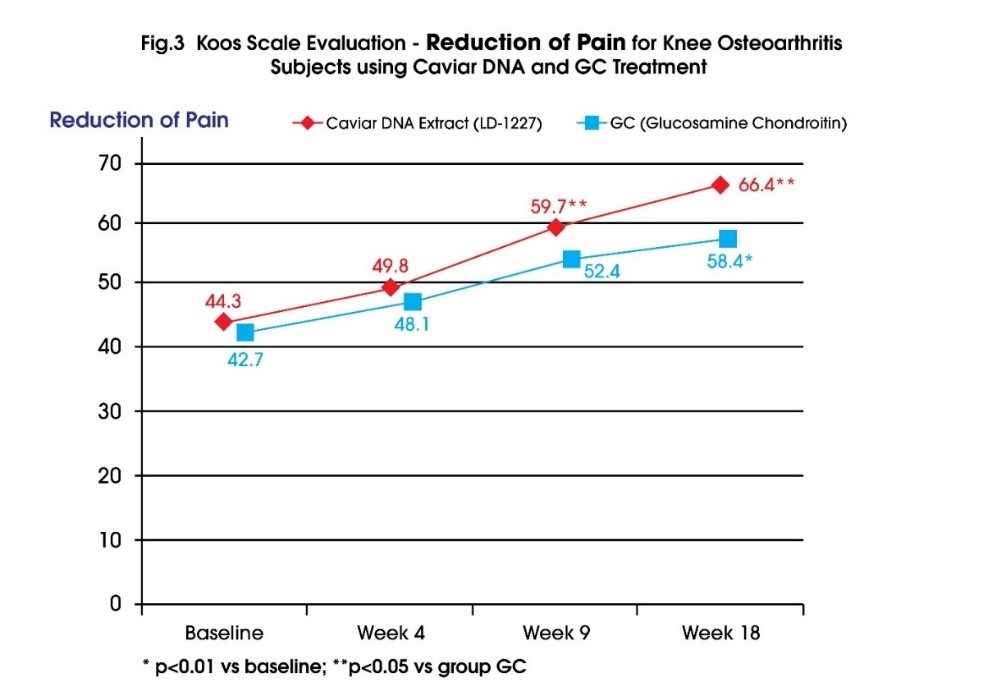
Figure 3 shows that once again that Caviar DNA extract (LD-1227) can help the reduction in pain and it is a outstanding option for pain management in the long term.
Note: KOOS (Knee disability and Osteoarthritis) score system is divided into 5 segments namely pain symptoms, function in daily living, function in recreation, other symptoms and quality of life.
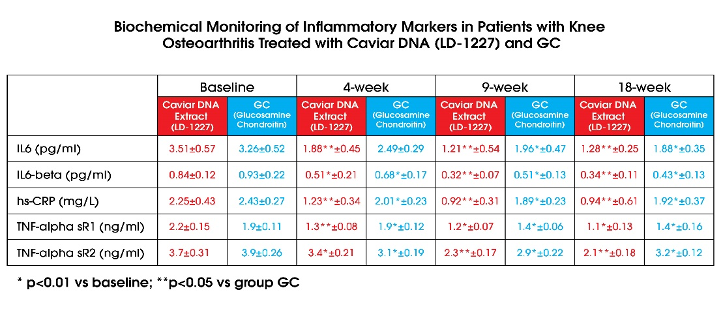
Biochemistry Analysis – Blood tests
Patients in the two groups were tested for inflammatory markers like Tumour Necrosis Factor Alpha, C Reactive Protein, Interleukin 6 etc, cytokines during the 18 weeks study period after taking the Caviar DNA extract (LD-1227) versus those taking GC.
Table 7 demonstrates that patients administered with Caviar DNA extract (LD-1227) have significantly Lower Inflammation over time as compared to GC. This implies that Caviarlieri can not only help to reduce joint pain over time but more importantly also to reduce chronic inflammation. This will enhance the recovery process for Osteoarthritis patients and thereby reduce pain.
- Empirical Randomised Double Blind Placebo Clinical Studies on Key Ingredients of Caviarlieri on Osteoarthritis
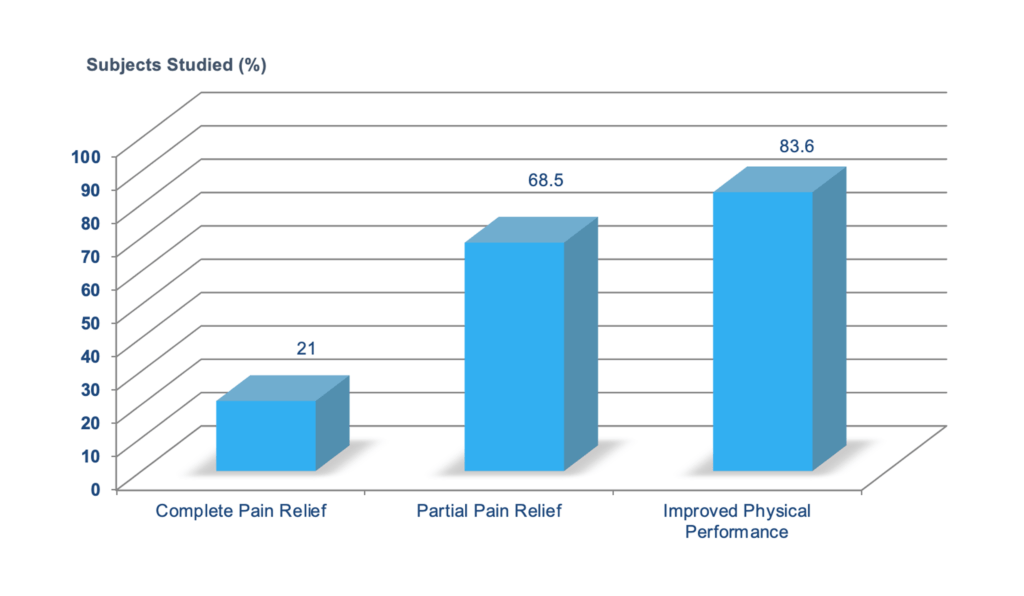
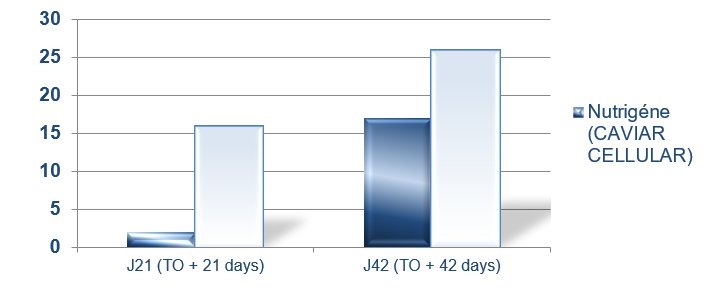
It is evident from this chart that the benefits of Caviar DNA Extract from Caviarlieri for joint pain management outweigh the use of painkillers over time.
Another study was done using the same combination (CAVIAR & MARINE Cellular DNA Complex, Vitamins A and E) to test against diclofenac (a steroidal anti-inflammatory) on a group of 67 fairly invalid volunteers who had hip or knee osteoarthritis. After 42 days of treatment, pain was reduced by 39%, and the impotent degree was reduced by 16, 1% with CAVIAR & MARINE Cellular DNA Complex (versus 35% and 26.1% respectively with diclofenac) (Figure 3).
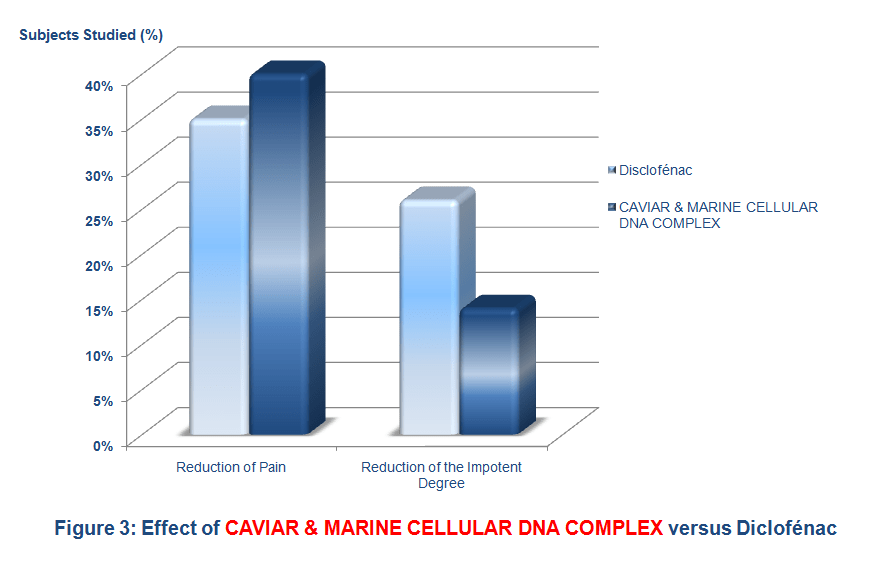
Conclusion: It is evident, from both the Caviarlieri scientific and empirical studies on the key ingredients of Caviarlieri, that there is consistency in terms of sustainable results and outcomes in significantly reducing joint pain, improving functional mobility and improving the quality of life for Osteoarthritis patients without adverse side effects over time as compared to taking opioids and NSAIDs.
Why is Caviarlieri a safe and potent option?

Caviarlieri is not a drug but an oral food supplement approved by the Swiss Public Health Authority. Unlike drugs or medications, there are no side effects for long term use. Caviarlieri is on Cologne List® and therefore undergoes independent quality checks. These are carried out by one of the globally-leading laboratories in nutritional supplement analytics for doping substances.
Subject
Recent Posts
-
The Amazing Benefits of Highly Polymerized Fish Collagen Peptides with Elastin – Caviarlieri
-
The World’s Most Effective Caviar DNA Extract with Marine Bioactive Peptides
-
Are Supplements effective for Joint Pain?
-
Why Is Sustainable Immunity Important for Your Long-Term Health
-
What is your “Body Age” – Biological Age?




